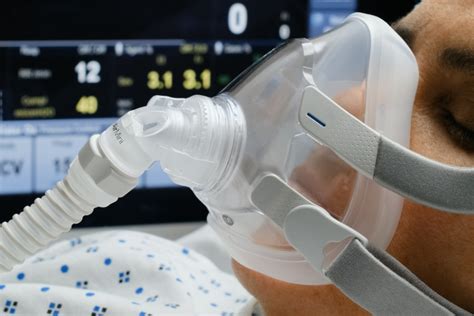
Breathing Support: Tools and Methods to Aid Respiratory Function
Breathing Support FAQ
How does pressure support help a patient breathe easier?
Higher levels of pressure support are used to help patients breathe easier by introducing positive pressure to supplement their spontaneous effort. PSV can be used as a stand-alone ventilation mode or as a weaning mode from mechanical ventilation.
How do pressure support levels affect the work of breathing?
Increased pressure support levels are introduced to alleviate the work of breathing (WOB) by supplementing the patient's spontaneous effort with positive pressure. When using pressure support levels between 10 and 12 mL/kg, the ventilator takes over all the WOB. Patients consistently govern breath frequency, duration, and flow in a PSV environment.
What devices are used in the ICU to help with breathing?
There are a variety of devices and machines that are used in the ICU to help with breathing. A nasal cannula is a simple tube that directs oxygen into the nose. This is the least amount of breathing support that a patient can use. Oxygen can be delivered with a face mask.
What support does a patient need in intensive care?
Most patients admitted to intensive care require some form of respiratory support. This is usually because of hypoxaemia or ventilatory failure, or both. The support offered ranges from oxygen therapy by face mask, through non-invasive techniques such as continuous positive airways pressure, to full ventilatory support with endotracheal intubation.
How can breathing control and breathing techniques help you?
The breathing control and breathing techniques on this page will help you to manage your breathing better. A worrying thought can make you feel anxious and make you feel breathless. This could make you feel panicked and bring on physical symptoms such as a tight chest or fast breathing.
What are the benefits of breathing exercises?
Breathing exercises offer many physical and mental health benefits. Discover three deep breathing techniques you can use to feel calmer. Whether you’re living with a heart condition, caring for someone who has one, or are concerned about having a heart problem in the future, it’s normal to experience stress.
How can breathlessness be managed?
Breathlessness can be managed using breathing techniques. You can also change the position you’re in to recover from breathlessness. What affects breathlessness?
How can i Improve my Breath?
This could be a slow walking programme, where you go at your own pace and rest when you need to, increasing the distance over time. Chair-based exercises to improve your posture can also help you breathe better. Sitting in a hunched-up position can make muscles tight, which makes breathing harder.
Breathing Support References
If you want to know more about Breathing Support, consider exploring links below:
What Is Breathing Support
- https://www.verywellhealth.com/what-is-intubation-and-why-is-it-done-3157102
- https://geekymedics.com/cpap-vs-niv-bipap/
- https://www.thoracic.org/patients/patient-resources/managing-the-icu-experience/breathing-support-for-respiratory-failure.php
- https://www.bmj.com/content/369/bmj.m2446
Breathing Support Information
- https://www.bhf.org.uk/informationsupport/heart-matters-magazine/medical/shortness-of-breath
- https://www.asthmaandlung.org.uk/symptoms-tests-treatments/symptoms/breathlessness/how-can-i-manage-my-breathlessness
- https://www.nhs.uk/mental-health/self-help/guides-tools-and-activities/breathing-exercises-for-stress/
- https://www.gosh.nhs.uk/conditions-and-treatments/procedures-and-treatments/continuous-positive-airway-pressure-cpap-non-invasive-ventilation/
- https://www.england.nhs.uk/long-read/adult-breathlessness-pathway-pre-diagnosis-diagnostic-pathway-support-tool/
- https://www.resus.org.uk/home/faqs/faqs-basic-life-support-cpr
Explore Related Topics
Creating a Sleep Sanctuary for Improved Diabetes Management
Share tips on setting up a conducive sleep environment to support diabetes treatment.
Sleep Quality and Diabetes: How does Holistic Sleep Hygiene Impact Blood Glucose Levels?
Discuss the importance of quality sleep in diabetes management
Sleep Hygiene and Diabetes Control: A Must-Know Connection
Delve into the relationship between quality sleep and diabetes management